
The 4 Levels of Structured Reporting in Radiology: A Framework for Enterprise Automation
For many years, structured reporting has been a goal in radiology to enhance report quality 1. However, clinical practice results have been inconsistent, with varying opinions regarding the impact of enterprise structured reporting solutions on productivity and quality.
Executive Summary: This article shares my experiences with structured reporting implementations. I use 'levels' of structured reporting to demonstrate why some are disappointed with the quality and productivity after implementation. I provide ways to guarantee improved quality and productivity in a structured reporting implementation.
| Reporting Level | Radiologist Efficiency | Data Integrity | Institutional ROI |
|---|---|---|---|
| Level 0: Free Text | Baseline | Low (high variability) | Baseline |
| Level 1: Standardized Layout | Small Impact | Medium (Improved compliance) | Small (+2-5% revenue) |
| Level 2: Structured Content | Medium Impact | High (clinical standardization) | Moderate |
| Level 3: Automated | Largest Improvement | Highest (Verified accuracy) | Maximum Potential |
The European Society of Radiology statement paper indicates radiologist Preston Hickey initially observed that variability in language and style prevented radiological reports from being used for further analysis 2[ESR]. Today, surveys identify key reasons for adopting structured reporting, as shown below 1[Academic Radiology]. Although radiologists hold mixed views on structured reporting, clinicians overwhelmingly prefer structured reports for readability 4[Radiology].
- Standardizing reporting styles (51%)
- Improving billing accuracy (36%)
- Reducing errors (35%)
- Enhancing resident education (34%)
- Streamlining reporting systems (25%)
Different Structured Reporting Levels
Martijn Nobel usefully characterized structured reporting as Level 1: Structured Layout and Level 2: Structured Layout with Structured Content5[Insights Imaging]. I expand Nobel’s characterization into four levels, as it provides insight into best practices and actionable data to improve efficiency and quality.
- Level 0. Free text
- Level 1. Standardized Layout
- Level 2. Standardized Layout and Structured Content
- Level 3. Standardized, Structured and Automated
Level 0 – Free Text Structured Reporting
Free text report templates are the original or conventional report templates. They are still used everywhere for rare or complex cases where less structure is a feature. Illustration 1 illustrates a Free Text PowerScribe template.
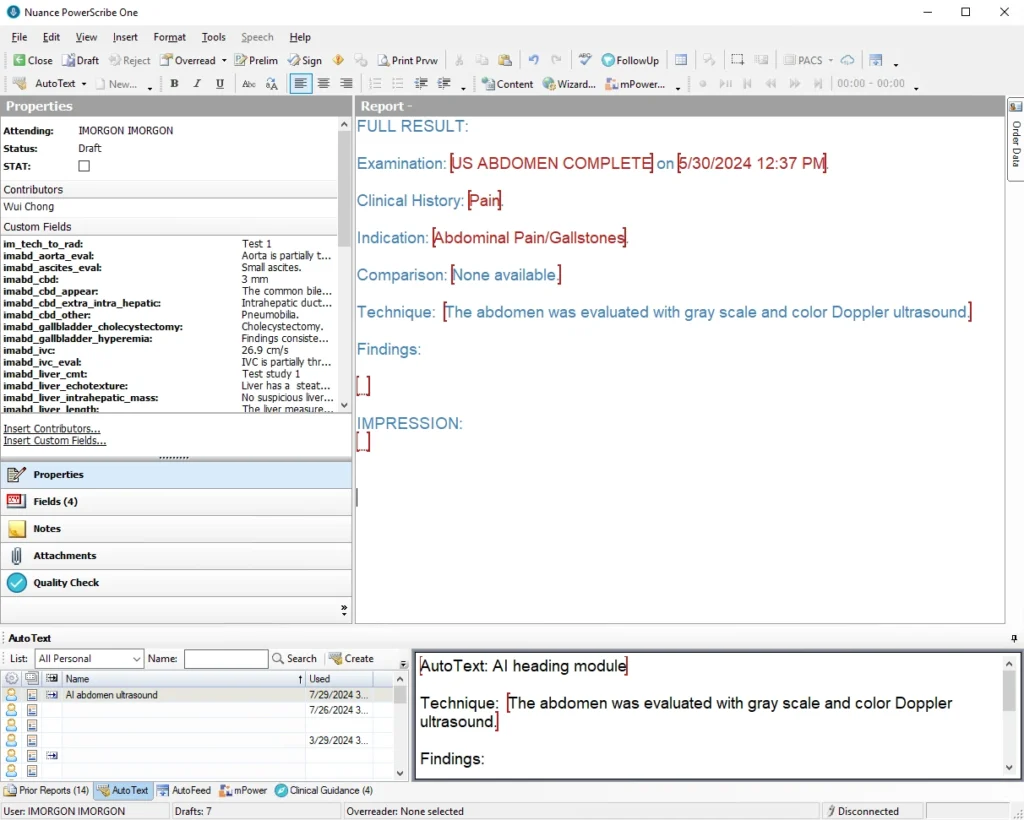
Level 1 – Standardized Layout Structured Reporting
A standardized layout ensures all essential elements are included. Early adopters and most (33%) of radiology reporting used standardized layouts1.
A primary motivation for a standardized approach is to maximize reimbursement. For instance, a complete abdominal ultrasound examination requires imaging of eight structures: the liver, gallbladder, bile ducts, kidneys, pancreas, spleen, inferior vena cava, and aorta. The incomplete report is re-coded as a limited abdominal examination if any of the eight elements are missing.
Reclassifying exams as limited is not uncommon, as estimates range from 9.3 to 20.2%, with a revenue loss of 2.5-5.5%7 [J Am Col Rad]. In one study, incomplete abdominal ultrasound reporting declined from 3.1% to 0.6% after implementing structured reporting7.
Many standardized layouts also prepopulate with ‘normal’ findings to reduce report generation effort.
While standardized layouts enhance consistency, they can introduce rigidity and inefficiency, especially for experienced radiologists 1.
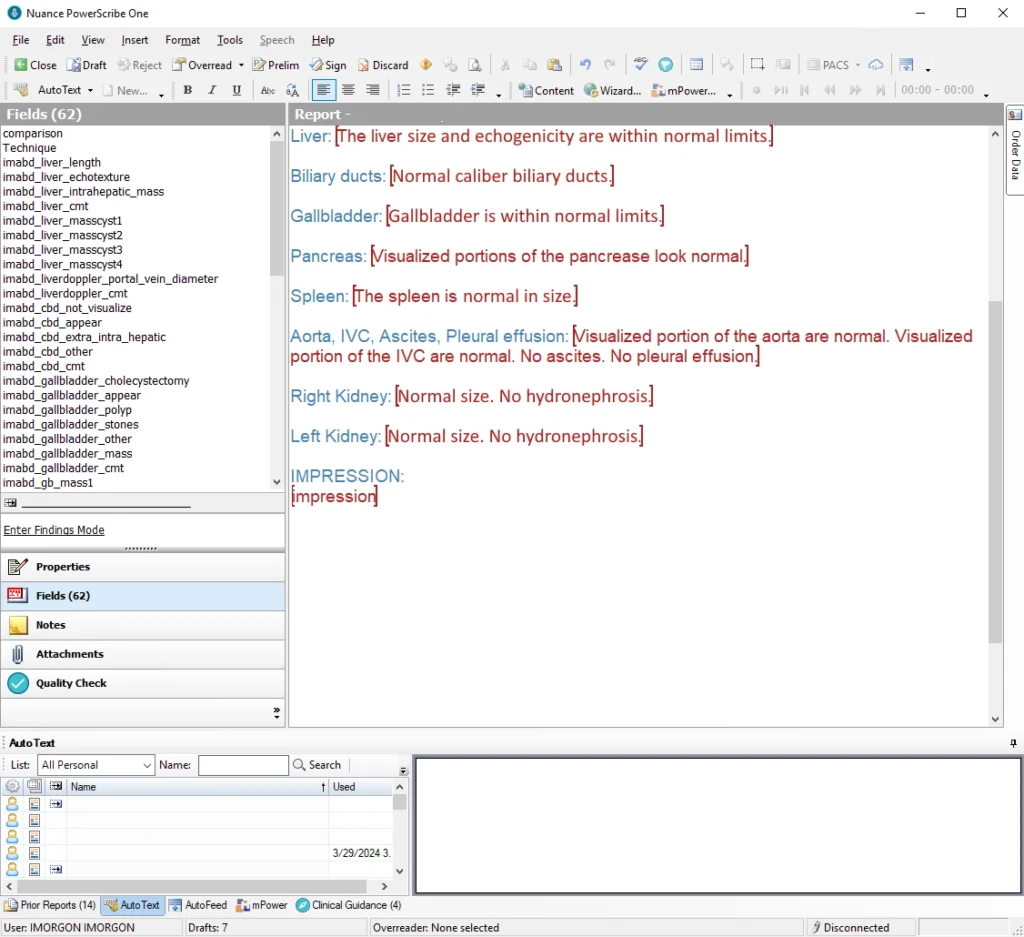
Level 2 – Standardized Layout AND Structured Content Structured Reports
Level 2 builds upon the standardized layout by incorporating structured content and organizing clinical information beyond organ-specific details5. Depending on the reporting tool (PowerScribe, Fluency, etc.), dropdown menus, picklists, and point-and-click functions supplement speech recognition to facilitate the insertion of routine, structured content.
Level 2 implementations are less common due to IT dependencies, particularly among non-technically proficient radiologists with limited free time.
One particular use of structured content is to support the implementation of clinical decision support systems, such as ACR TI-RADS or LI-RADS. These systems further standardized data and content through clear definitions, specific terms, grading systems, or point systems. However, anyone who has implemented these tools can attest to the significant shortcomings of common reporting tools such as Nuance PowerScribe when handling complex ACR TI-RADS or O-RADS scoring.
As with Level 1, efficiency and rigidity can pose challenges for experienced radiology reporters. Interestingly, structured content was occasionally associated with less accurate reports when inappropriate ‘normal’ template text was not deleted or modified.
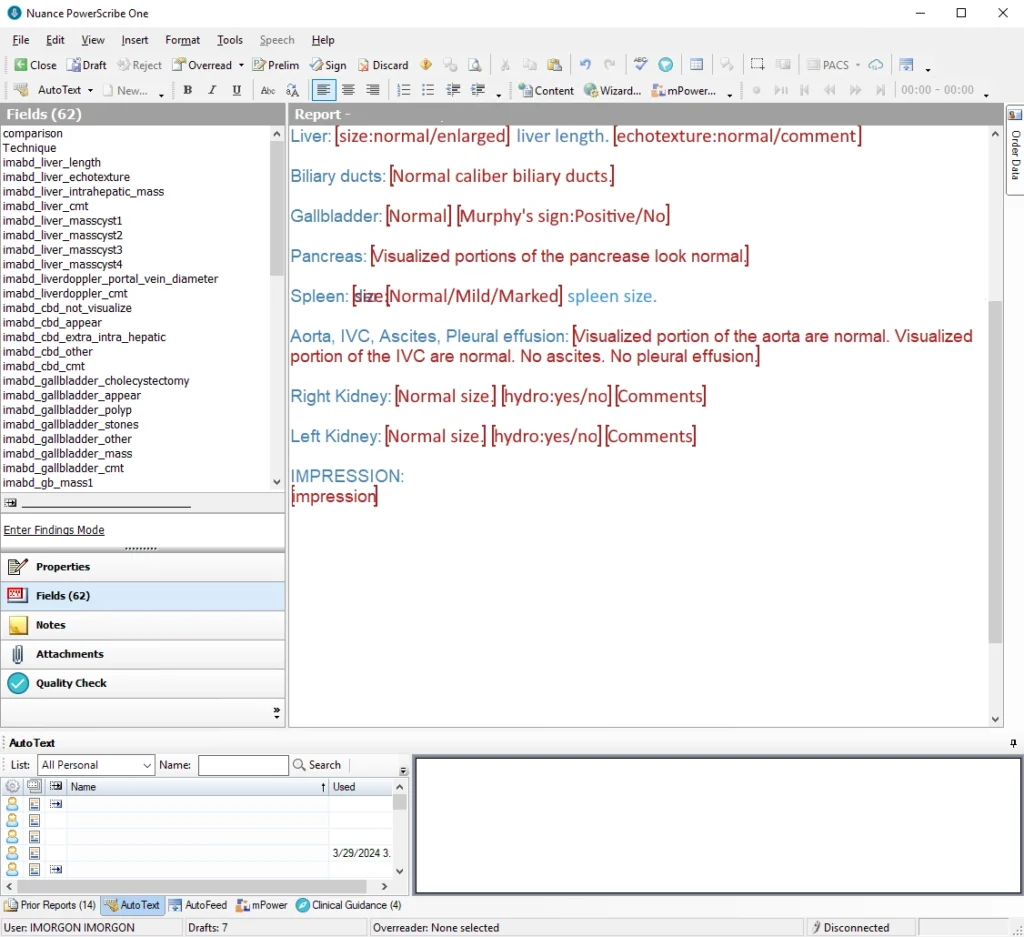
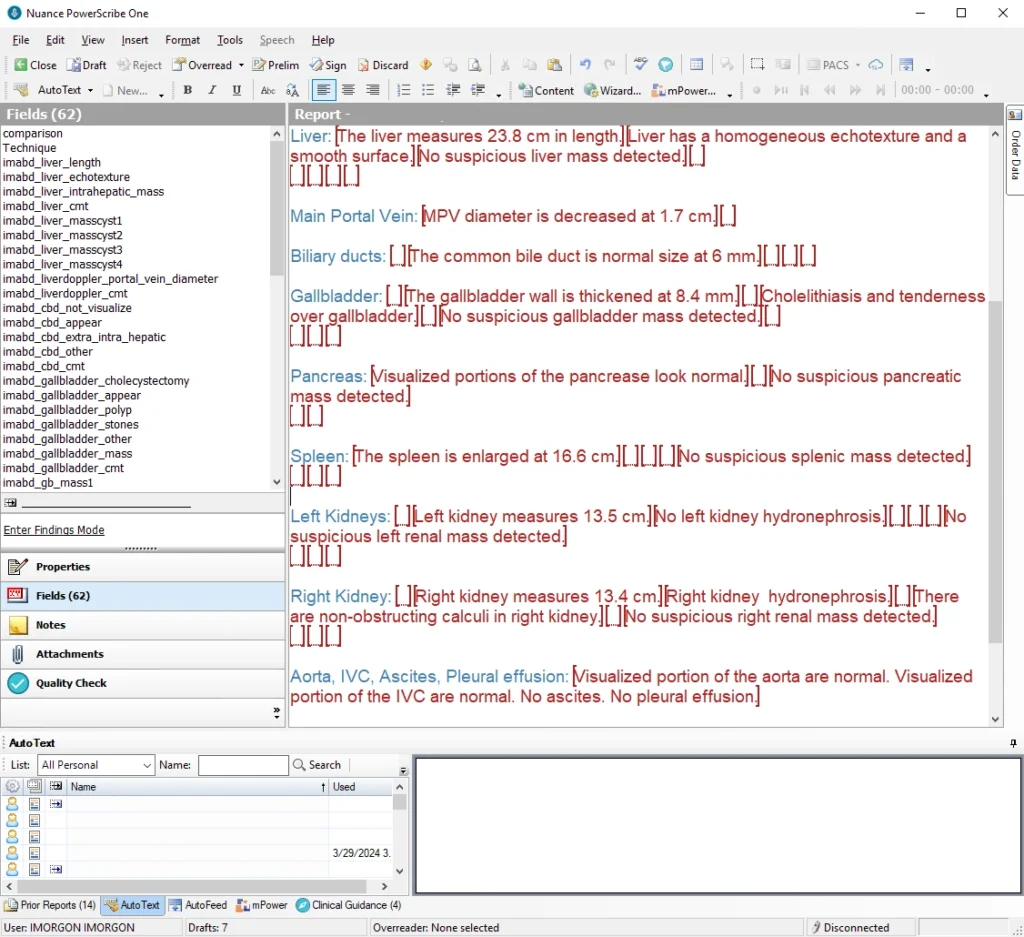
Level 3 – Standardized, Structured, and Automated Structured Reporting Solution
Level 3, Automation, builds on the standardized template and structured content to prefill Findings and some Impressions, creating a draft report. Automation is in addition to macros and picklists in Level 2. In academic settings, residents or fellows often serve as manual ‘automation’ tools to create draft reports 😭.
However, dedicated software has emerged to automate the creation of ‘preliminary’ reports.
A large opportunity in ultrasound exists because sonographers scan patients and complete worksheets to cover qualitative data. With the right tools, extracting relevant information from sonographer measurements and worksheets enables automated preliminary report generation—a sonographer can provide the same ‘automation’ as the resident or fellow. Also, with the right tools, this requires less effort than traditional methods such as paper worksheets and scanning. This Level 3 automation is why we created our enterprise ultrasound reporting software.
Measurement-only solutions
Many sites implemented ‘partially automated’ solutions. These sites use applications from Modlink or Laurel Bridge to transfer DICOM SR measurement data to the reporting program. My previous article [50% of fields are Qualitative] found 50% of fields in report templates are ‘qualitative’ versus quantitative (measurement) information11. Qualitative information encompasses echogenicity, the presence of gallstones, and Murphy’s sign. One point of the blog was that a measurement-only solution does not achieve the productivity and quality of a Level 3 implementation because it addresses only half of the template fields.
AI, DEXA, CT and other Modalities
Although ultrasound is most commonly used for reporting automation, the second most frequently used modality is DEXA. DEXA is a more straightforward implementation because it requires no worksheets for qualitative information. Automation is also possible in 3D labs, where technicians perform segmentation and measurement tasks. Coronary calcium scoring is a sample opportunity that comes to mind.
There has been a steady increase in the use of artificial intelligence applications for image analysis to generate report content. These AI tools are often limited to a specific clinical application and research settings. Regardless, AI tools can be combined with specialized radiology reporting software to automate the drafting of all reports in an imaging department.
Imorgon Solution
Imorgon can improve every healthcare organization’s clinical practice reporting process to Level 3. It overcomes the limitations of auto-text and picklists in existing reporting packages. Imorgon eliminates the need to transcribe measurements and most qualitative data. Features enabling this include:
- Integrated Clinical Decision Support calculators, eliminating web lookups
- Automatic retrieval of prior measurements and radiological reports
- Drawings with automatic measurements
- Calculators for volumes and interval differences
- Enhanced pick lists with enhanced conditional text generation
- Integrated logic to prevent contradictions or highlight exceptions
Imorgon also ensures the successful implementation of reporting automation through:
- Enforcement of best practices through webforms/worksheets
- Measurement data mapping with guaranteed data transfer
- Template development assistance
- 24×7 support
Imorgon tools will generate a completed draft radiological report. Imorgon can improve quality and productivity and achieve a very high ROI in radiology reporting.
Though outside the scope of this article, Imorgon also ensures successful implementation through Institutional Governance, Epic integration, 24/7 technical assistance, and guaranteed mapping.
Conclusions for a Structured Reporting Solution
Imorgon has the experience to implement and support any initiatives. If your facility uses free text, a standardized layout, or even basic measurement transfer software, Imorgon will improve your workflow and quality of care.
References
- Powell DK, Silberzweig JE. State of structured reporting in radiology, a survey. Acad Radiol. 2015 Feb;22(2):226-33. doi: 10.1016/j.acra.2014.08.014. Epub 2014 Oct 23. PMID: 25442793. ↩︎
- European Society of Radiology (ESR). ESR paper on structured reporting in radiology-update 2023. Insights Imaging. 2023 Nov 23;14(1):199. doi: 10.1186/s13244-023-01560-0. PMID: 37995019; PMCID: PMC10667169. ↩︎
- Powell DK, Silberzweig JE. State of structured reporting in radiology, a survey. Acad Radiol. 2015 Feb;22(2):226-33. doi: 10.1016/j.acra.2014.08.014. Epub 2014 Oct 23. PMID: 25442793. ↩︎
- The Radiology Report as Seen by Radiologists and Referring Clinicians: Results of the COVER and ROVER Surveys Jan M. L. Bosmans, Joost J. Weyler, Arthur M. De Schepper, and Paul M. Parizel
Radiology 2011 259:1, 184-195 ↩︎ - Nobel, J.M., Kok, E.M. & Robben, S.G.F. Redefining the structure of structured reporting in radiology. Insights Imaging 11, 10 (2020). https://doi.org/10.1186/s13244-019-0831-6 ↩︎
- Powell DK, Silberzweig JE. State of structured reporting in radiology, a survey. Acad Radiol. 2015 Feb;22(2):226-33. doi: 10.1016/j.acra.2014.08.014. Epub 2014 Oct 23. PMID: 25442793. ↩︎
- Pysarenko K, Recht M, Kim D. Structured Reporting: A Tool to Improve Reimbursement. J Am Coll Radiol. 2017 May;14(5):662-664. doi: 10.1016/j.jacr.2016.10.016. Epub 2016 Dec 24. PMID: 28027857. ↩︎
- Pysarenko K, Recht M, Kim D. Structured Reporting: A Tool to Improve Reimbursement. J Am Coll Radiol. 2017 May;14(5):662-664. doi: 10.1016/j.jacr.2016.10.016. Epub 2016 Dec 24. PMID: 28027857. ↩︎
- Powell DK, Silberzweig JE. State of structured reporting in radiology, a survey. Acad Radiol. 2015 Feb;22(2):226-33. doi: 10.1016/j.acra.2014.08.014. Epub 2014 Oct 23. PMID: 25442793. ↩︎
- Nobel, J.M., Kok, E.M. & Robben, S.G.F. Redefining the structure of structured reporting in radiology. Insights Imaging 11, 10 (2020). https://doi.org/10.1186/s13244-019-0831-6 ↩︎
- Surprising Improved Productivity with Ultrasound Worksheets (imorgon.net) ↩︎
